
You are what you eat. This is true in so many ways, yet nutrition was not taught to me in medical school. It took me ten years of clinical practice to learn about the complexity of nutrition and its effect on our health. What I’d like to discuss in part 2 is what happens to our health when our digestive processes are disrupted. But first, back to June.
One of the interesting tidbits of information I learned during her intake evaluation was that for several years prior to her first visit with me she had experience gas and bloating while eating grains and even noticed undigested food in her stool from time to time. These symptoms slowly worsened over several years. She didn’t realize the relationship of these symptoms with her allergies because her allergies had been going on for years prior to her gastro symptoms. By the time her hands started to become stiff and achy, she had just considered her allergies and gut symptoms as unrelated nuisances. It wasn’t until a few year later when the diarrhea started that she decided to seek medical attention for her gut symptoms. No one asked her about her eating habits and she never bothered to mention her allergies. It wasn’t until her life was disrupted that she began to understand something was happening with her health. The first practitioner she saw told her she had IBS and she could take a prescription antispasmodic medication for her symptoms. When this didn’t help, she saw another doctor, who performed a colonoscopy and told her she was fine. She bounced from practice to practice all the while her diarrhea steadily worsened. She did notice some relief when she went ‘Paleo’ for a while, but all her symptoms returned when she went back to her usual diet and no one could tell her why her symptoms went away and then returned.
What I’d like to discuss today is what happens when the digestive process is disrupted and what symptoms and diseases are associated with these disruptions.
The model used by Functional Medicine educators for this is DIGIN:
Digestion/Absorption
Digestion first starts in the oral cavity and continues through the stomach and small bowels. This requires hydrochloric acid, enzymes, and bile production at the right place and at the right time.
Hydrochloric Acid
Many individuals won’t produce enough hydrochloric acid for a myriad of reasons. This could be due to age (acid production decreases as we age), stress (we produce 25% of our digestive enzymes just by relaxing and smelling/seeing our food), antacid medications (Prilosec OTC), chronic illness (like diabetes or heart disease) or nutritional deficiencies.
The decrease in stomach acid can have the following consequences:
- Small Intestinal Bacterial Overgrowth (symptoms of carbohydrate intolerance + immediate bloating)
- Dysbiosis (overgrowth of intestinal bacteria)
- Chronic yeast overgrowth
- Mineral deficiencies (Ca, Mg, Zn, Fe, Cr, Mo, Mn, Cu)
- B12 deficiency
- Bloating or belching immediately following meal
- Feel like food sits in stomach
- Dilated capillaries in face (acne rosacea)
- Multiple food allergies
- Post adolescent acne
This decrease in stomach acid has also been associated with the following diseases:
Addison’s • Asthma • Autoimmune disease • Celiac disease • Dermatitis herpetiformis • Diabetes • Eczema • Gallbladder disease • Graves’ disease • Hepatitis • Chronic hives • Lupus erythematosus • Myasthenia gravis • Osteoporosis • Pernicious anemia • Psoriasis • Rheumatoid arthritis • Rosacea • Sjogren’s syndrome • Thyrotoxicosis • Hyper- and hypothyroidism • Vitiligo
It’s amazing to see how many different symptoms and differing diseases are associated with decreased stomach acid. There are several ways that stomach acid production can be supported. These include digestive enzymes, betaine HCL, Swedish bitters, stress management, and slowed eating. We will dive into this more in part 3.
Digestive Enzymes
The next major elements needed for proper digestion are the digestive enzymes produced by the pancreas. It releases its content into the first part of the small bowel to meet the yellow acidic fluid (called chyme) that exits the stomach. The pancreatic secretions neutralize the stomach acid and continue the digestive process. Pancreatic secretions contain the following enzymes:
- Lipases: break down fats
- Proteases: break down proteins
- Amylases: break down carbohydrates
Pancreatic insufficiency is common enough that the FDA has approved a medication called Creon to treat this entity. This insufficiency can be caused and exacerbated by inflammatory food, inhibitors in foods, chronic stress, toxins, alcohol abuse and nutritional insufficiencies.
Bile Production
The final part of this triad is bile production. This process starts in the cells of the liver. Small ducts carry the bile produced in the liver to its storage tank, the gallbladder. When food is eaten, at the right time under the correct environment, the gallbladder will contract and release its contents into the small intestine together with the enzymes from the pancreas. These bile salts are responsible for emulsification or breakdown of digested fat into small globules or fat balls. Low levels of bile production result in poor digestion of fat containing foods, diarrhea, fat vitamin deficiencies (Vitamins A/D/E/K) and fat in the stool. If you have had your gallbladder removed, then odds are you will have some sort of digestive issue related to its loss.
There are many foods and products that can improve bile production and secretion, these include:
- Radishes (horse, red, daikon)
- Dandelion, chicory, other bitter greens
- Bile salts (ox bile) 500–1000 mg with food
Intestinal Permeability (aka ‘Leaky Gut’)
The next level for digestive disease is with a disruption in Intestinal Permeability, the second part of DIGIN. The technical term for this is increased gastrointestinal permeability, but it is commonly referred to as ‘leaky gut.’ The cells that line your small intestine were designed to only let certain molecules pass and keep the unwanted contents of the bowel in the lumen. This process requires an intact mucous layer, tightly bound cells and a functional cell surface-lumen interface. When these three processes are disrupted, leaky gut ensues.
A disruption of any previous digestive processes can contribute to this as well as direct interactions with chemicals in our food. For example, emulsifiers used in food production can emulsify the protective mucous lining found in the small bowel. Commonly used emulsifiers in modern food production include mustard, soy and egg lecithin, mono- and diglycerides, polysorbates, carrageenan, guar gum and canola oil. In excess these can contribute to leaky gut. Food chemical and environmental toxins can also disrupt the balance of this barrier.
Increased gastrointestinal permeability, or leaky gut, has been associated with the following diseases:
Acute pancreatitis • Asthma • Autism • Autoimmune hepatitis • Autoimmune disease • Bechet’s disease • Burn patients • Celiac Disease • Chronic Fatigue Syndrome • Eczema • Food Intolerances • Fibromyalgia • IgA nephropathy • Inflammatory bowel diseases • Irritable Bowel Syndrome • Kidney Stones • Migraines • Multi-Organ Failure • Multiple sclerosis • Non-Alcoholic Liver Disease • Primary biliary cirrhosis • Primary sclerosing cholangitis• Psoriasis
The following is a listing of potential treatments for this breakdown in the gut lining and barrier:
- Elimination Diet/Avoidance of provoking foods and substances
- Bone Broths and Vegetable Broths
- Glutamine: 1000–30,000 mg daily in cold or cool beverage
- Zinc: 25–50 mg daily
- Colostrum: 1000–3000 mg daily
- Quercetin 500–1000 mg 3–5 x daily
- Proteolytic enzymes
- Bromelain 250–500 mg
- Stinging nettles 300 mg daily
- Butterbur
- Probiotics 10–100 billion CFU daily
- Fiber: Larch bark
- Vitamin A: 10,000–30,000 IU daily for 30 days
- Aloe Vera
Gut Microbiota
The Gut Microbiota is the next level of dysfunction in the DIGIN mnemonic to address when attempting to fix your gut. Commonly called dysbiosis, this is simply an imbalance in the composition of bacteria found in the colon. Each person’s microbiota is so individualized that it can be used like a fingerprint to identify someone but the composition of one’s microbiota is not as important as the functions it performs. It regulates our overall health and metabolism; it can affect our mood and food choices. Certain yeast produce compounds call pseudo neurotransmitters that activate feeding centers in the brain and stimulate our cravings for carbohydrates to feed the yeast in our colon. It becomes a vicious cycle.
Microbiome research has shown its disruption associated with the following diseases:
• Atopic illnesses • Autoimmune Diseases • Cardiovascular disease • Dermatologic issues • Diabetes • Digestive Health • Mental illnesses such as schizophrenia • Obesity • Pain
There is even a specialized test call DayTwo that measures the DNA of the microbiome and based on its composition, dietary changes to feed different bacteria have been showed to help loose weight and regulate diabetics sugar levels. The image below shows a schematic of the effects on diet on the microbiome and how it affects health.
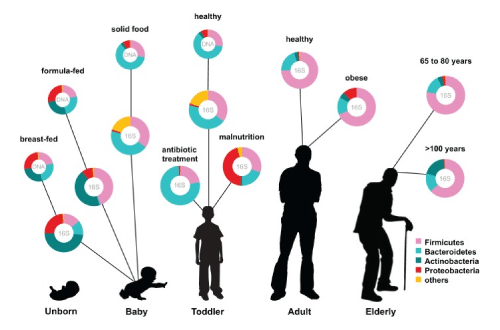
The major leverage point for changing the microbiome is diet. Foods rich in fiber and specialized non digestible sugars are key here. Below is a listing of a few of these:
• Jerusalem artichokes • Onions • Chicory • Garlic • Leeks • Bananas• Fruit
• Soybeans • Burdock root • Asparagus • Maple syrup/sugar • Chinese chives • Peas • Legumes • Eggplant • Honey • Green Tea• Yogurt, cottage cheese, kefir
Inflammation
Inflammation is the next level in DIGIN to address when working on GI tract health. This can be evaluated by advanced functional stool testing. Typically, the inflammation is related to disruption of the microbiota in the gut as well as activation of the immune system related to all the topics we have previously covered. Treatment here is focused on the type of inflammation discovered as well as the disruption in the gut bacteria that testing reveals as well as digestion and nutritional issues that are uncovered. Addressing the DIG in DIGIN typically lowers the inflammation. In fact, 80% of our immune system surrounds the GI tract and its activation can cause a host of food reactions, food sensitivities as well as system wide inflammation.
Though not delving deep into this topic here (inflammation is addressed in another of our blog series), it is critically important.

The major leverage point for changing the microbiome is diet. Foods rich in fiber and specialized non digestible sugars are key here. Below is a listing of a few of these:
• Jerusalem artichokes • Onions • Chicory • Garlic • Leeks • Bananas• Fruit
• Soybeans • Burdock root • Asparagus • Maple syrup/sugar • Chinese chives • Peas • Legumes • Eggplant • Honey • Green Tea• Yogurt, cottage cheese, kefir
Nervous System
The nervous system in the GI tract is robust. There are as many neurons in the GI tract as there are in your spinal cord and there is a specialized connecting system related to the vagus nerve that connects the GI tract to the brain. This was recently discovered and discussed in this article in Science from 2018.
Eighty percent of the activity between the GI tract and brain is from the GI tract TO the brain, NOT vice versa. So, some of the newer thinking is that the gut has a more profound impact on brain health than the brain does on the gut. Addressing gut health through the process outlined here can have a profound impact on mental health and function. Newer research is now even showing that Parkinson’s Disease begins in the neurons of the GI tract decades prior to its diagnosis.
What’s Next?
In part 3, I will discuss a treatment plan aimed at working through the above and addressing your gut health and ultimately your entire bodies health.
Since 2010, Richmond Integrative and Functional Medicine has been helping people to restore their health and hope with an integrative approach to conventional and alternative medicine that’s entirely science-backed. We at RIFM believe everyone is made for health. We offer a comprehensive, in-person patient membership program to ensure you get access to the care you need to thrive.




