When I first encountered Fibromyalgia (FM) and Chronic Fatigue Syndrome (CFS) during my medical training in the late 90’s, I was informed they were psychiatric conditions treated with antidepressants. Typically (but not exclusively) occurring in females, these conditions were difficult to diagnose and equally difficult to treat. Most Fibromyalgia and Chronic Fatigue Syndrome patients I saw visited several prior specialists and came with a bag filled with prescription medications, none of which were very effective. These were the difficult patients I would cringe to see—knowing I had little to offer them—yet their stories were long and filled with emotion and I wanted to help. I still want to help, and thankfully, I now believe I can.
What I’d like to do first in this two part series is to explain Fibromyalgia and Chronic Fatigue Syndrome from a Functional Medicine Perspective. Then, in part II I will discuss functional medicine treatment options for fibromyalgia.
Part One:
What are FM/CFS?
So, what exactly are Fibromyalgia and Chronic Fatigue Syndrome (FM/CFS)?
The short answer is we still don’t know. The long answer is the following: A syndrome is a constellation of symptoms that together, without any definitive cause, is labelled a syndrome. Once the definition is made, scientists are enabled to begin to research it and clinicians to diagnose it. But syndromes change. For example, Down’s Syndrome used to fit this category but once the Trisomy 21 gene mutation was discovered we had an exact cause, and a new name. Irritable Bowel Syndrome is currently undergoing the same transition. We now know some IBS-D and Mixed Type are a low grade inflammatory condition and there is now a test for them through Quest Labs (anti-cytolethal distending toxin B and anti-vinculin). The syndromes of Fibromyalgia and Chronic Fatigue Syndrome are likewise experiencing this transition and our understanding of them is changing constantly.
The History of FM/CFS
In the late 1800’s, Chronic Fatigue Syndrome was known as neurasthenia, which literally means ‘weak nerves.’ Teddy Roosevelt developed this condition and was advised to withdraw from the business of society and into the serenity of nature, later to regain his vigor and return to his active life. There is considerable overlap with so-called ‘adrenal fatigue’ due to both having HPAG Axis dysfunction, but Fibromyalgia and Chronic Fatigue Syndrome is more global and includes ‘adrenal fatigue’ within its’ scope.
There is considerable overlap with so-called ‘adrenal fatigue’ due to both having HPAG Axis dysfunction, but CFS/FM is more global and includes ‘adrenal fatigue’ within its scope.
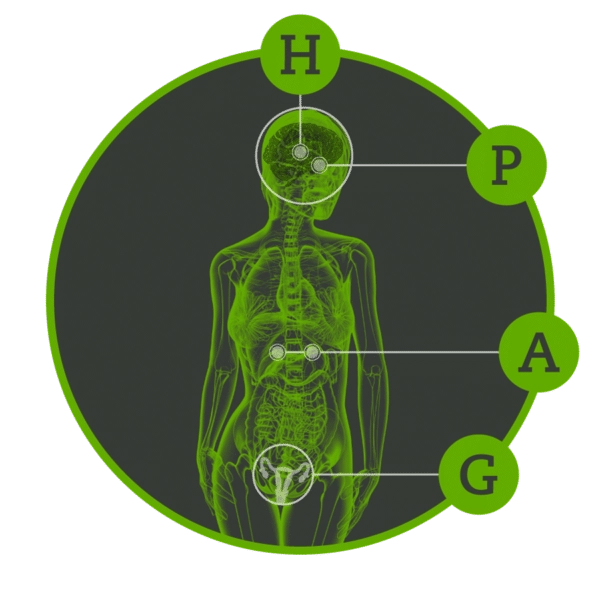
(hypothalamus, pituitary, adrenal, gonadal axis)
By the close of the twentieth century, Fibromyalgia and Chronic Fatigue Syndrome was thought to be primarily a psychiatric illness and was treated with antidepressant and mood stabilizing/seizure meds. But research originating from Massachusetts General in 2015 gave us the first evidence that Fibromyalgia and Chronic Fatigue Syndrome has a brain based inflammatory component to it. This brain based disorder results in a general dysregulation in the patient’s HPAG Axis (hypothalamus, pituitary, adrenal, gonadal axis?—?see figure 1).
But what sets up individuals for this condition?
Fibromyalgia and Chronic Fatigue Syndrome Causes
Imunal
One such cause is brain-based neuroinflammation—primarily situated in the microglia of the brain. In other words, immune cells in the brain are overactive. The result is HPAG Axis dysfunction that causes a system wide ‘energy crisis.’ This is a treatable condition if you can determine the root cause and then address the system wide dysregulation that has led up to the neuroinflammatory energy crisis.
Sleep
Another related cause is chronic sleep disturbances. Disrupted sleep is known to cause chronic fatigue as well as immune system suppression and disrupt neurotransmitter levels. In Shift Sleep Work Disorder, patients present with non-restorative sleep, irritability and depression, chronic fatigue, difficultly thinking and low testosterone levels. Newer research is associating things ranging from increased risk of breast cancer to diabetes with this condition. We are just beginning to learn how important sleep is for our overall health and wellbeing.
Functional Medicine Recommendations For Better Sleep
Viral Infections
Viral infections are another less known cause for chronic fatigue syndrome. The Epstein Barr Virus was one of the first infections associated with chronic fatigue syndrome. Now there has been described a post-Lyme Syndrome associated with chronic fatigue syndrome and chronic yeast overgrowth. In these conditions, immunologic markers are abnormal. For example, it is typical to see an elevated C4a level and/or a depressed Natural Kill Cell (CD57) level.
Chronic fatigue syndrome and Fibromyalgia also affects cell function though limiting some of the primary energy sources for the cell, the most important one being ATP. Recent metabolic studies have shown the following in Fibromyalgia and Chronic Fatigue Syndrome patients:
- ATP in neutrophils is lower
- Lower levels of ATP in platelets
- Reduced ATP and creatine in muscles of Chronic Fatigue Syndrome patients
- Lower blood levels of NADPH
- Elevated cytokine levels (i.e.inflammatory markers)
What this means is that for some reason our bodies ability to recycle and regenerate ATP is limited at the minutest level of the cell. NADH is a carrier for energy and creatine is an important energy form in muscles.
We could continue to list associated conditions and presumed antecedents here (e.g. micronutrient deficiencies, toxin exposures, heavy metal exposures) but you get the idea. Many differing causes over the span on one’s life can lead up to the singular entities of Fibromyalgia and Chronic Fatigue Syndrome.
The Perfect Storm
The perfect storm for the rapidly increasing incidence of this condition can now be seen more clearly. The unhealthy practices of our modern society combined with the above exposures set us up for the growing epidemic. The following is small listing of contributing factors:
- 50% of the typical American diet’s diet consists of empty calories, lacking nutrients
- Average sleep in US has dropped from 9 hours pre-1900 to 6.5 hours today
- Falling hormone levels of both aging males and female (too detailed to discuss here)
- Increase in chronic stress and chronic/recurrent low-grade infections
- Increased toxin and chemical exposure (average infants placental blood tests positive for 200+ chemicals)
- Multiple nutrient deficiencies: 80% of Americans are magnesium deficient and 60% are deficient in any single B vitamin
Hypothalamic dysfunction and decreased energy production are hallmarks of chronic fatigue syndrome and fibromyalgia, the hypothalamus is the center of our sleep/wake cycles, temperature regulation, autonomic function (i.e.-blood pressure maintenance and digestive function), pain response and hormone levels just to name a few. The insults listed above over time can wreak havoc on your brain, centering on the HPAG axis. For this part of the brain to work properly, a lot of energy in the form of ATP is needed. The human brain uses about 30% of our consumed calories. Muscle function as well requires large amounts of ATP, it requires more ATP for muscles to relax than to contract.
With the dysfunctions and insults above, the symptoms of chronic fatigue syndrome and fibromyalgia become evident:
- Exhaustion
- Achiness
- Weight gain
- Brain fog
- Increased thirst
- Low blood pressure
- Blood pressure fluctuations
- Sexual dysfunction
- Disordered sleep
- Non-restorative sleep
- Bowel dysfunction
- Irregular hormone levels
- Irritability
- Mood swings
- Depression
- Anxiety
- Recurrent infections
- Pain/tactile sensitivity
Hopefully the above is a clear explanation of Chronic Fatigue Syndrome and Fibromyalgia from a functional medicine doctor. Below/Attached is a short form questionnaire meant to help you see what systems may be involved and as a help to your personal health care practitioner.
In Part II, I will discuss treatment options that you can discuss with your personal licensed health care practitioner.