Chronic Lyme | Part 2
Beyond Antibiotics
Why Treating Lyme Requires More Than Killing Bacteria

Aaron Hartman MD
January 21, 2026

Subscribe
Never miss out on new content from Dr. Hartman.
If Lyme disease is caused by bacteria, then antibiotics should fix it, right?
 That logic makes sense. It’s the model most people are given, and for some patients, it works well enough. Acute infection is identified early, treated appropriately, and symptoms resolve.
That logic makes sense. It’s the model most people are given, and for some patients, it works well enough. Acute infection is identified early, treated appropriately, and symptoms resolve.
But that’s not everyone’s experience…
For a significant (and growing) number of patients, symptoms persist long after antibiotics are finished. Fatigue, pain, cognitive changes, sleep disruption, mood instability. Often with normal or inconclusive lab work. Often with growing frustration.
This is where the conversation around Lyme becomes polarized. Either antibiotics are treated as the only answer, or they are dismissed entirely.
Neither position reflects what actually happens in complex cases. The truth lives in the middle.
Antibiotics Are a Tool, Not a Strategy
In my recent conversations with Veronica Porterfield, PA-C  , this distinction came up repeatedly.
, this distinction came up repeatedly.
Antibiotics can reduce bacterial load. They can be an important part of care. But they do not address everything Lyme disrupts in the body.
As Veronica put it plainly:
We’re not anti-antibiotic. We’re anti-oversimplification.
That sentence matters.
When antibiotics are treated as the entire plan, rather than one tool within a broader strategy, patients are often set up for disappointment. Not because antibiotics failed, but because expectations were misaligned with biology.
Why Killing Bacteria Is Not the Same as Restoring Health
By the time Lyme becomes chronic, the problem is rarely just the presence of bacteria.
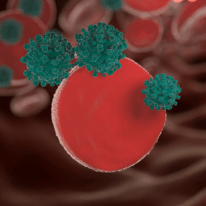 It’s the body’s response to that presence over time.
It’s the body’s response to that presence over time.
In Article 1, we talked about terrain. Here, that concept becomes practical.
Persistent Lyme often involves:
- immune systems that are exhausted, suppressed, or misfiring
- inflammatory signaling that no longer shuts off appropriately
- detox pathways that are overwhelmed
- nervous systems locked in vigilance
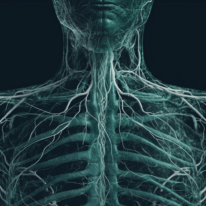 Antibiotics do not reset those systems. They cannot tell the immune system how to recalibrate. They cannot restore mitochondrial resilience. They cannot calm a nervous system that has been on high alert for months (or years).
Antibiotics do not reset those systems. They cannot tell the immune system how to recalibrate. They cannot restore mitochondrial resilience. They cannot calm a nervous system that has been on high alert for months (or years).
So even when bacterial burden is reduced, symptoms may persist.
That’s not imaginary. It’s physiology.
Biofilms & Why Treatment Can Stall

One of the most important concepts Veronica emphasized in our discussions was biofilms.
Biofilms are protective structures that bacteria use to survive hostile environments. They are not unique to Lyme, but they are highly relevant to it.
Inside a biofilm, bacteria are:
- harder for antibiotics to reach
- less visible to the immune system
- metabolically different than free-floating organisms
This matters because antibiotics are most effective against actively dividing bacteria. When organisms shift into protected or dormant states, the rules change.
Veronica described it this way:
You can throw antibiotics at something the body can’t see and the immune system isn’t coordinating with.
That doesn’t mean nothing is happening, but it does mean progress can be limited.
Biofilms are one reason treatment can feel like it hits a wall. Not because the wrong drug was chosen, but because the context was incomplete.
When Treatment Makes People Feel Worse
 Another common experience in Lyme care is symptom flares during treatment. Patients often interpret this as harm or failure. Clinicians sometimes do too.
Another common experience in Lyme care is symptom flares during treatment. Patients often interpret this as harm or failure. Clinicians sometimes do too.
But in many cases, what is happening is immune activation.
As bacterial load shifts, inflammatory signaling increases. Detox pathways are stressed. Cytokines rise. The nervous system reacts.
This can feel frightening if no one has explained it.
Veronica framed it carefully:
A flare doesn’t automatically mean treatment is wrong. Sometimes it means the immune system is finally engaging, but the body doesn’t yet have the capacity to handle the byproducts.
This is why pacing matters. It’s also why treatment sequencing matters.
Why Sequencing Changes Everything
One of the most consistent themes in our conversations was sequencing.
Not everything should be done at once. Not every system can be pushed simultaneously.




In complex Lyme cases, clinicians often need to:
- reduce toxin burden before aggressive antimicrobial work
- support detox and elimination pathways early
- stabilize sleep and blood sugar
- calm nervous system reactivity
If you don’t reduce the total load first, the body stays in survival mode. You can’t force healing on a system that’s just trying to get through the day.”
This mirrors what we discussed earlier this month in The 3 Types of Stress. Lyme is a form of biochemical stress, but it rarely exists alone. Physical and emotional stressors compound it.
Antibiotics address one piece. Sequencing addresses the whole.
Why Tests Don’t Always Tell the Whole Story
Another source of confusion for patients is testing.
Some people are told they no longer have Lyme because a test is negative, even though symptoms persist. Others never test positive despite clear clinical patterns.
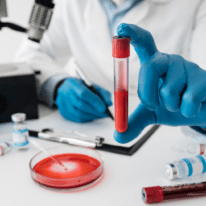 That doesn’t necessarily mean the tests are unreliable. But current tests are limited.
That doesn’t necessarily mean the tests are unreliable. But current tests are limited.
In late 2025, the U.S. Department of Health and Human Services convened a national roundtable to discuss gaps in Lyme diagnostics and clinical care, emphasizing the need for improved detection and better support for patients with persistent symptoms.
That recognition matters because it validates what patients and clinicians have been observing for years:
- A negative test does not always equal resolution.
- A positive test does not explain everything.
Clinical context still matters.
A Broader Definition of Progress
 One of the traps patients fall into is defining progress too narrowly.
One of the traps patients fall into is defining progress too narrowly.
If the only marker of success is symptom disappearance, any fluctuation feels like failure.
In complex Lyme cases, progress often looks like:
- better sleep before less pain
- more stable energy before cognitive clarity
- fewer crashes before sustained improvement
These shifts indicate that systems are recalibrating, even if the process is not linear.
As Veronica reflected:
“People want a straight line. Healing is almost never a straight line.”
That uncertainty is hard. But it’s also honest.
Where This Leaves Patients
 If antibiotics alone have not resolved symptoms, it does not mean:
If antibiotics alone have not resolved symptoms, it does not mean:
- you waited too long
- you failed treatment
- Lyme is untreatable
It usually means the strategy needs to expand.
A systems approach does not reject antibiotics. It contextualizes them. It recognizes that restoring health requires supporting the immune system, reducing load, and rebuilding resilience.
That’s not a shortcut. But it is a more realistic path.

Antibiotics can kill bacteria. Healing requires more than that.
It requires understanding how Lyme reshapes the immune system, the nervous system, and the body’s capacity to recover. It requires sequencing rather than intensity. It requires addressing load, not just pathogens.
When we stop asking why antibiotics failed and start asking what the body still needs, the conversation changes.
And for many patients, that change is where progress finally begins.
